If you’re looking to find out more about the CSPs role in shaping community rehabilitation and recovery services across the UK, then look no further

Here you’ll find all the information you need about how the CSP is ensuring equitable access to high-quality, person-centred rehabilitation and recovery services, based in the community.
Rehabilitation and recovery services make people’s lives better, yet many of those who could most benefit face barriers to accessing them. We want to change that.
Rehab champions
The CSP's rehab champions in parliament support the #RightToRehab and help us to campaign for policy and legislative change.
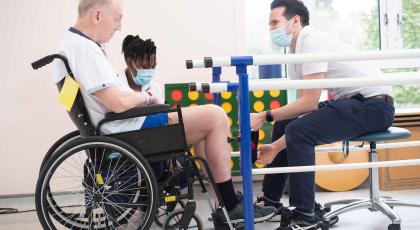
The human impact of community rehab and recovery
Discover the real-world consequences of high-quality community rehabilitation and recovery services when they are available, and when they are not.
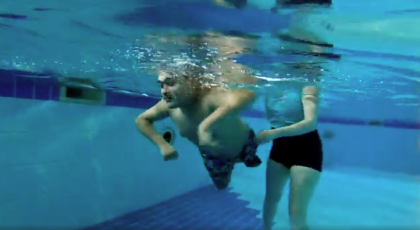
Why community rehab and recovery matters
We already know that rehabilitation works and that more needs to be based outside hospitals, in the community, closer to home.
But to do this, we need to reshape services, and overcome long-standing challenges.

Alliances working across the UK
We are continuing to build alliances across the UK, committed to lobbying to improve access to quality rehab and recovery services across the UK.

Important reading
We’re dedicated to improving the quality of rehabilitation and recovery services, and know this must be underpinned by evidence.

How to influence decision makers
If we’re to reshape and improve community rehabilitation and recovery services, then we can’t do it alone.
Here’s how you can champion community rehab and recovery with local healthcare decision makers

Loss of rehab space
Find out how you can take action if your service is impacted by loss of physiotherapy space and download and personalise our template letter, which you can use to raise the issue directly with your trust's chief executive.

Collaborate, don't compete
How collaborative working with other exercise professionals can improve outcomes for patients, populations and communities

Recovering from the Covid-19 pandemic
Thousands of people across the UK need rehabilitation and recovery after covid.
Our healthcare system, too, needs to recover.

Intermediate care framework and community rehabilitation model FAQs
The FAQs set out here are designed to help CSP members and other AHPs better understand what the Intermediate Care Framework (ICF) and new model for rehab mean for them.





































