Physiotherapists in Blackpool are leading the use of lung ultrasound within the respiratory physiotherapy profession, following the introduction of a unique training programme.
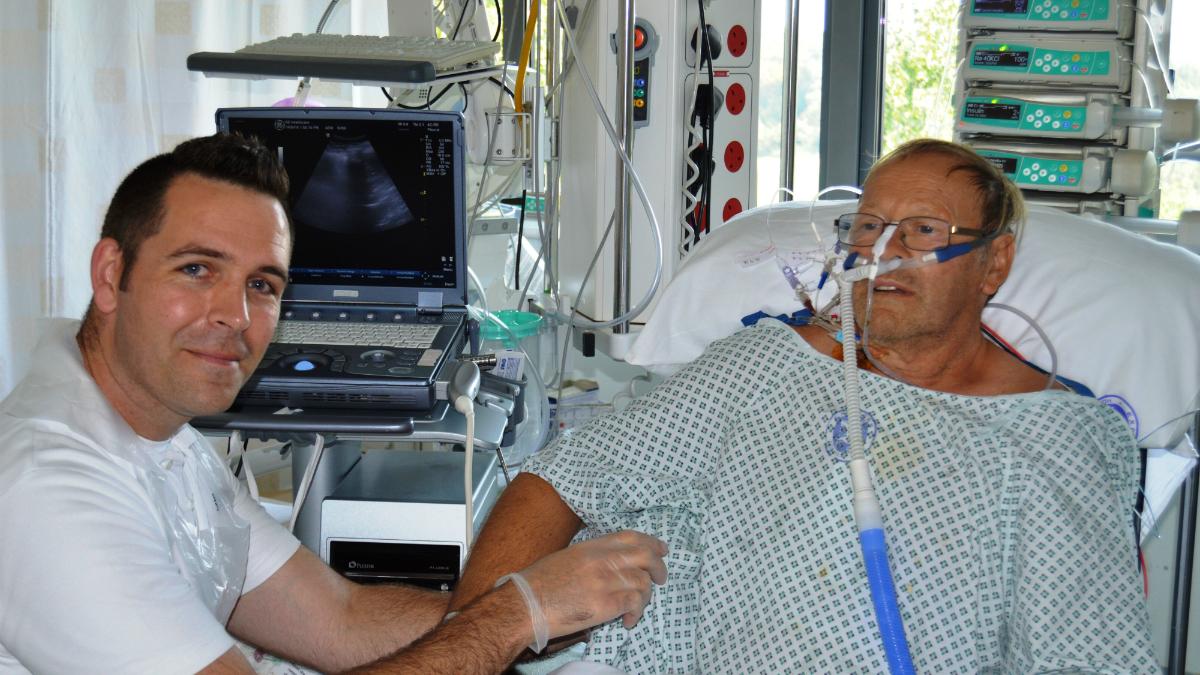
The initiative at Blackpool Victoria Hospital, part of Blackpool Teaching Hospitals NHS Trust, has led to a new lung ultrasound function within the physiotherapy department–which the trust claims is the first of its kind in the UK.
Three physiotherapists at the hospital are now fully qualified to use the imaging technique, which can help diagnose many lung conditions, and nine more physios are currently undergoing training.
Simon Hayward, a critical care physio at the hospital, is the driving force behind the scheme. Since 2013, he has been using lung ultrasound to help inform his treatment options, and he became the first physiotherapist to gain the Intensive Care Society’s core ultrasound intensive care (CUSIC) accreditation in 2016. Since then he has become a CUSIC mentor and has helped to organise a specially designed training programme for his physiotherapy colleagues.
‘The training includes an introductory course that covers physics, probe handling, pathologies and image acquisition and interpretation,’ he said.
‘And trainees also undertake supervised scans, independent scans to build a logbook, and a triggered assessment to show competency.’
As a result, two of his colleagues have now gained CUSIC accreditation, and the long-term aim is to provide training to all the senior respiratory physiotherapists within the trust by the beginning of 2020.
‘That would enable lung ultrasound to be provided across critical care, surgery, acute medicine, paediatric and cystic fibrosis services,’ he explained.
Diagnostic benefits
Mr Hayward believes lung ultrasound offers a number of advantages in comparison to other imaging techniques.
‘On a chest X-ray conditions such as consolidation, pleural effusion, blood in the plural cavity and collapsed lung all look white - everything that has any sort of density just looks white,’ he said.
‘But with lung ultrasound you can start to differentiate between fluid and solid tissue or between air and even slightly different densities of tissue – so you can tell if you are looking at a pure pleural effusion or blood.’
In addition, the technique allows treatments to take place while scanning a patient.
‘So you can see how it’s affecting the person there and then, which chest X-rays and MRI can’t do.’
And it can be performed in real-time, at the bedside, without exposing patients to ionising radiation.
Improving patient care
Speaking about the technique’s benefits, Mr Hayward said ‘One patient was scanned by us four times in a day following the development of a serious lung condition.
‘The lung ultrasound scans allowed us to guide both medical and physiotherapy treatments to reverse this patient’s deterioration.’
Meanwhile, on another occasion, a lung ultrasound scan clearly highlighted a developing pneumonia when a patient’s chest x-ray had been clear.
‘Our patient was deteriorating and requiring more respiratory support, but it was unclear what the cause was,’ said Mr Hayward.
‘As soon as I scanned his lungs, I could see the signs of a chest infection on his left side.
‘He was started on antibiotics immediately and a chest x-ray the following day showed a significant left sided consolidation consistent with pneumonia.
‘In both these cases the patients had faster and more accurate treatment thus avoiding the need to be placed on a ventilator.’
Introductory course
Mr Hayward is also running a one-day ‘Introduction to lung ultrasound’ course at the hospital, which aims to offer physiotherapists who work in respiratory specialities a better understanding of the tool.
He said: ‘I believe lung ultrasound has made me a better physiotherapist. I can treat my patients more effectively and believe this technique is too important not to share with my fellow respiratory physiotherapists.'
Physiotherapists who would like more information about the introductory course can contact Mr Hayward at: simon.hayward1@nhs.net
Number of subscribers: 2



































