Physiotherapists, and other healthcare practitioners, should be able to use tools that help them identify people who are nearing the end of their life.

This is according to new guidance about the service delivery of end of life care from NICE, the National Institute for Health and Care Excellence.
It states that people who manage and deliver services should make use of tools, such as the Gold Standards Framework, the Amber Care Bundle or the Supportive and Palliative Care Indicators Tool, to identify people who are likely to be approaching the end of their life.
NICE says this could enable health and social care practitioners to start discussions about advance care planning, provide necessary care and appropriately support people's preferences for how they would like to be cared for and where they would like to die.
AGILE, the CSP professional network of physiotherapists specialising in the care of older people, welcomed the recommendations but emphasised a need for adequate training.
Sarah De Biase, chair of AGILE, said: ‘It is encouraging that this guidance highlights the approach and tools which health and care professionals may consider using to identify people at end of life.
‘However, from an implementation perspective, training and education needs to accompany the guidance to ensure that those using the tools are competent and confident in having conversations with people about end of life care and are supported to redesign systems within their organisations to allow these conversations to happen over time.’
The benefits of early identification

‘It is not always easy to identify when someone may be in the last year of their life,’ Ms De Biase said.
‘But the benefits of recognising when someone might be approaching their last year are many.’
The benefits can include:
- enabling someone to live well until they die by avoiding crisis and unnecessary hospitalisation or treatment burden
- supporting individuals to remain in their preferred place of care up to and at the end of their life
- empowering individuals to make informed decisions about how they would like to be cared for and what treatments they would be/not be willing to receive
- equipping carers with the information they need to support their loved ones as they die whilst looking after themselves
Involving carers in end of life conversations

The guidance also states that people approaching the end of their life should be given a chance to talk about their treatment plans with a healthcare professional, and be able to invite their carers, or other people who are important to them, to take part in these discussions.
Ms De Biase explained that discussions about end of life needed to be ‘dynamic’ and reviewed over time, as the needs and wishes of individuals - and their carers – might change as a person’s health deteriorated.
‘We need to support people and their loved ones to think and talk about dying and to prepare for dying,’ she said.
‘This is essential, and could help to minimise distress to carers and individuals at the end of life, for example through effective information provision about what to expect and/or trigger access to carer support services.’
Reducing unnecessary treatments
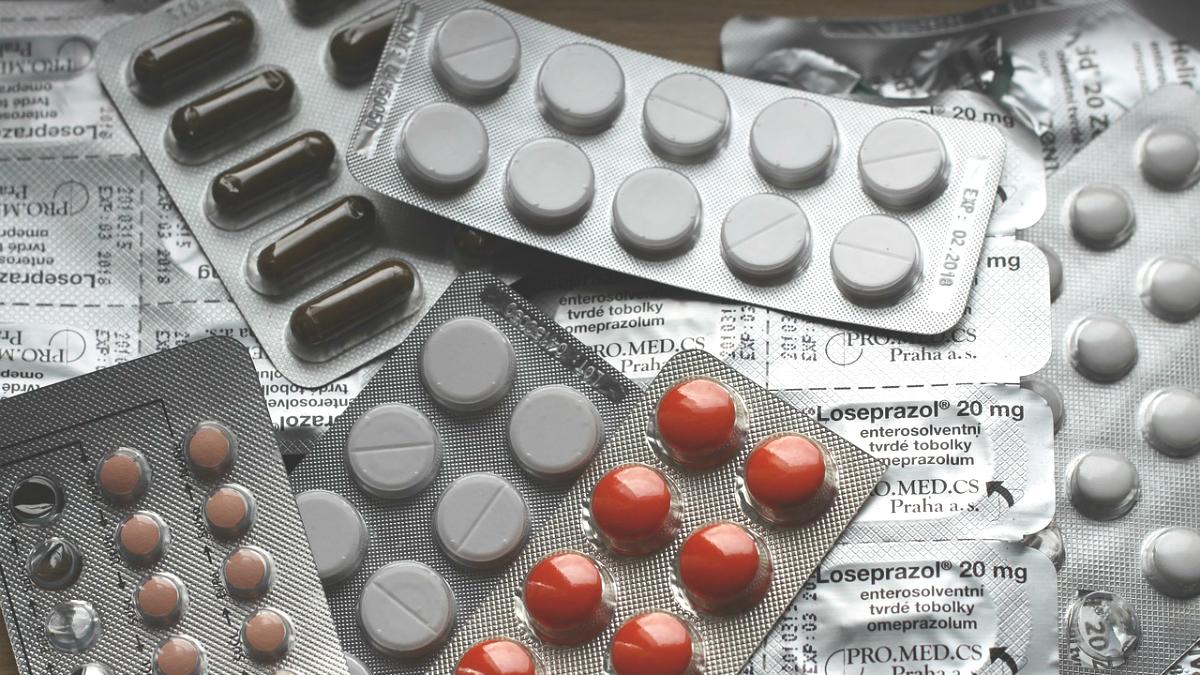
The new guidance also suggests that services should work together, sharing information about treatment reviews, in order to reduce the burden of unhelpful treatments.
‘This is a must,’ said Ms De Biase.
‘Many older people take more than four medications, but when they are approaching the end of their life many of these drugs will no longer be clinically effective and should be stopped.
‘However, we still see patients at end of life who are on large quantities of medication. This guidance should give physiotherapists confidence to hold others to account in the presence of unnecessary drug burden; and some physiotherapists, who are non-medical prescribers, may have a direct role in reducing unnecessary or harmful medication.’
Advance care planning
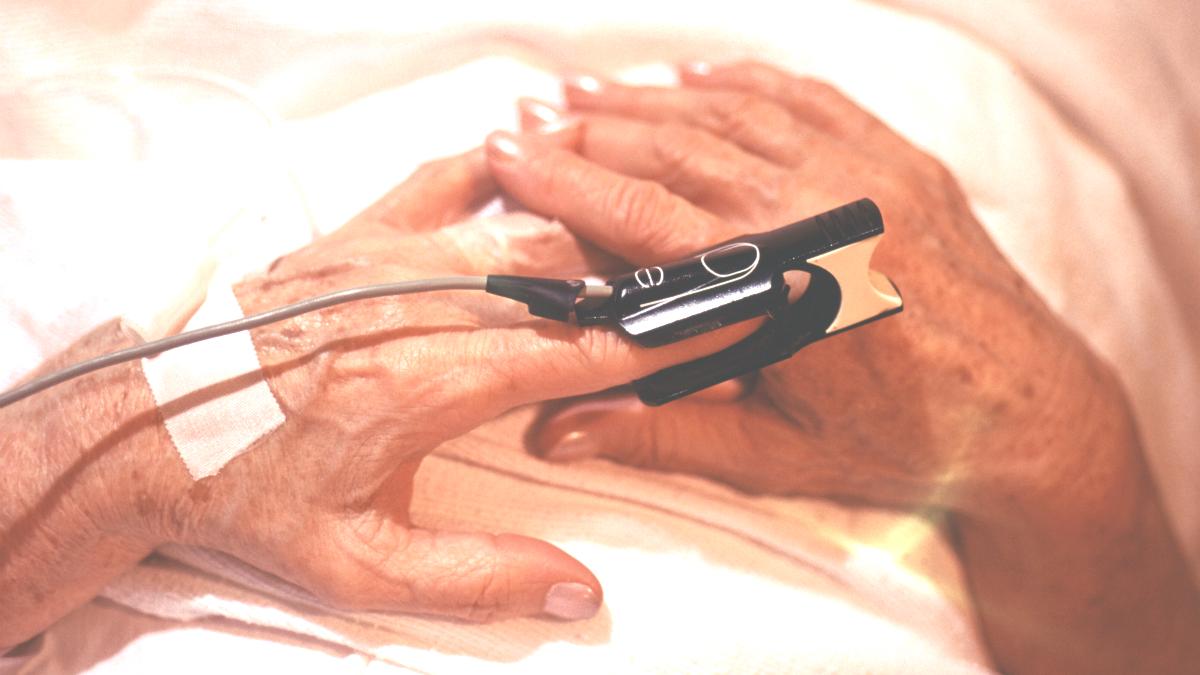
In addition, the guidance suggests that service providers develop policies to ensure that Advance Care Planning (ACP) is offered to all adults as they come close to the end of their life.
Ms De Biase described well delivered ACP as ‘a golden thread’ that was required to make end of life care ‘truly person-centred’.
‘We need to see more ACP leads at a place level and physiotherapists are well placed to fulfil such roles,’ she said.
She added that improving communication and information sharing between services was key to delivering effective ACP.
Early referral research
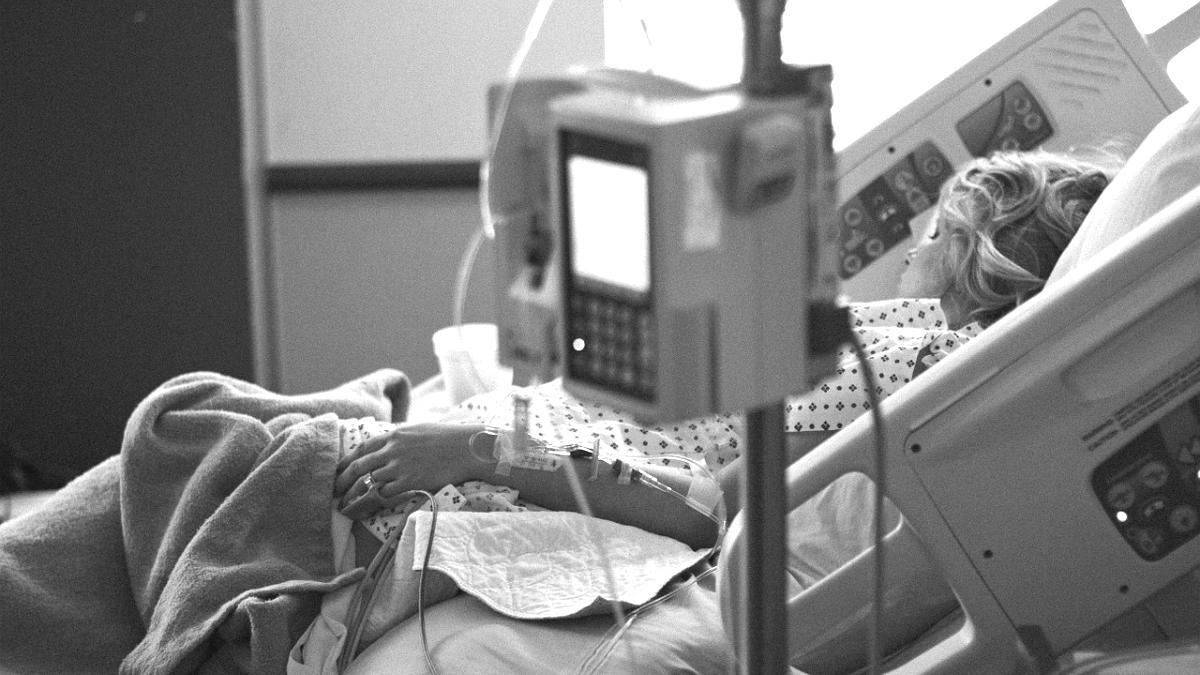
The guidance outlines four key research priorities, one of which highlights a need to study if outcomes for people nearing the end of their life can be improved by an early review of service provision and early referral to specialist palliative care services.
‘This priority has the potential to make the most difference for older people and their carers,’ said Ms De Biase
‘There is such a large body of evidence which demonstrates the value of early referral to palliative and/or support services for people who may be in their last year of life.
‘Not only do people report higher quality of life (even though they are dying), but the research also highlights people actually live longer when palliative care forms part of their multidisciplinary care and support.
‘At the AGILE annual conference in Northern Ireland in early October Prof Brian Dolan of the #last1000dayscampaign was our key note speaker – and our job now as physiotherapists is to be instrumental in the effective implementation of the new end of life care NICE guidance if we, as a profession, are to help people spend as few days in hospital as possible in their last 1000 days of life.’
Find Out More
Number of subscribers: 2



































