People with chronic post-operative neuropathic back or leg pain should have access to high-frequency spinal cord stimulation, along with appropriate multidisciplinary support and assessment.
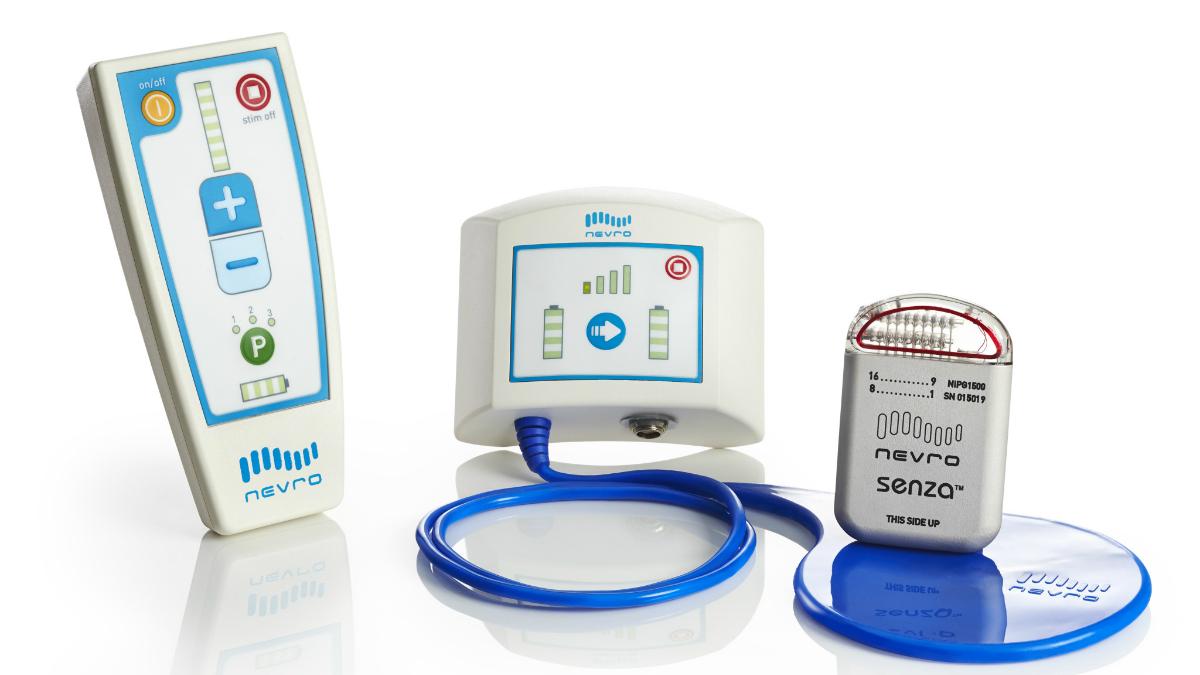
This is according to new guidance from the National Institute for Health and Care Excellence (NICE) which also recommends the use of the Senza spinal cord stimulation system.
Published last month, the guidance says Senza, which delivers high frequency therapy, should be considered as a treatment option for people with chronic leg or back pain that has not improved after surgery.
The high-frequency treatment requires a patient to have a small, battery-powered generator implanted under their skin. Clinicians then place electrodes, which connect to the generator, near the patient’s spinal cord The electrodes deliver high frequency (10kHz) electrical pulses which can alleviate the patient’s pain.
Diarmuid Denneny, chair of the Physiotherapy Pain Association and physio lead at University College London Hospitals’ pain management centre, told Frontline: ‘I work in a specialised pain service where we use spinal cord stimulation and high-frequency treatments.
‘The use of these devices is becoming more and more popular, but they are very expensive and it’s helpful if physios can be alert to unintended effects, for example on people’s activity and function, because if a person’s pain reduces they may immediately return to doing things in a normal way and then discover that they’re struggling.
‘From a physiotherapy perspective, there is a lot we can do to help patients with these implants, such as ensuring they receive appropriate pain self-management and guidance alongside the high-frequency treatment.’
Multidisciplinary support maximises impact
NICE says evidence backs the use of the Senza system for patients who are experiencing residual chronic neuropathic back or leg pain at least six months after back surgery, and despite conventional medical management.
It emphasises that patients who receive the treatment need to undergo a successful trial of stimulation as part of a wider assessment by a multidisciplinary team.
Mr Denneny added: ‘Where I work, we have set up a perioperative pain management programme that includes multidisciplinary input from physiotherapists, psychologists, nurses and other clinicians.
‘Having that wide range of support helps patients to develop a variety of self-management strategies that complement and hopefully maximise the impact of these devices.’
Find Out More
Number of subscribers: 4



































