A review concludes that targeting at-risk patients for breathing training before major surgery may reduce serious post-operative lung complications
Why was this study needed?
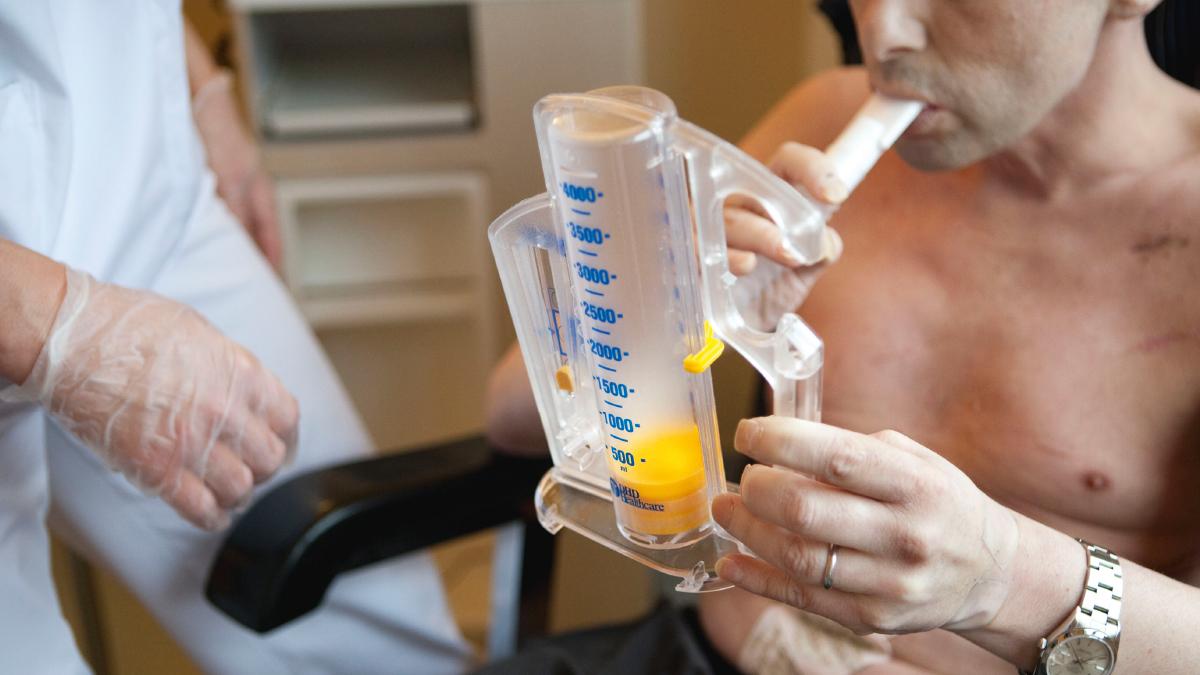
After major abdominal or heart surgery, people can experience a number of complications. These include lung infections (pneumonia), areas of collapsed lung from plugs of secretions in the airways, constricted airways or fluid in or around the lung. These may lead to respiratory failure (where the lungs cannot get enough oxygen into the blood stream). Such complications are associated with higher healthcare costs, longer stays in hospital, on-going illness and death. Prior to surgery people identified as being at risk can perform exercises supervised by a physiotherapist – called respiratory rehabilitation – designed to reduce the risk of complications. Inspiratory muscle training, which helps to strengthen the muscles around the lungs, is one example of a respiratory rehabilitation technique. This Cochrane review evaluated the effectiveness of inspiratory muscle training in people undergoing heart or major abdominal surgery, compared with usual care (such as advice on deep breathing exercises), a non-exercise intervention or no intervention. Trials of both low (i.e. healthy) and high risk participants were included. The risk factors that were reported in the trials included smoking, chronic obstructive pulmonary disease, diabetes, hypertension, and raised body mass index.
What did this study do?
This systematic review compared the results of 12 randomised controlled trials including 695 patients. Ten of the trials used a device that provides steady resistance against a breath in. Two trials used a threshold device in conjunction with exercise training, such as diaphragm strengthening. One trial compared a threshold device, deep-breathing exercises and incentive spirometry, which measures lung capacity and provides feedback.
This review followed the Cochrane Collaboration’s high methodological standards. Nine studies had a high risk of bias related to a lack of blinding – whether patients and staff were aware of the treatment received – but when researchers re-ran their analysis without these studies it did not affect the main findings. There was also a risk of selective reporting of outcomes in 11 studies. Overall across all studies the authors reported a risk of bias from the small number of patients included (small studies tend to overestimate the effects of an intervention).
What did it find?
The trials included adult patients with varying levels of risk and using differing definitions of risk. Outcomes also varied between studies, so the authors considered three complications that were consistently defined: atelectasis (volumes of collapsed lung), pneumonia and mechanical ventilation for over 48 hours.
Pooled results of seven trials showed that the breathing training significantly reduced the risk of collapsed lung (risk ratio [RR] 0.53, 95 per cent confidence interval [CI] 0.34 to 0.82) compared with usual care or no exercise. However, this evidence was judged low quality because the studies were small and may have had a risk of publication bias.
Eleven trials showed a reduction in post-operative pneumonia (RR 0.45, 95 per cent CI 0.26 to 0.77); this evidence was judged to be moderate quality as although the studies were small their quality was upgraded to moderate as there was a large effect.
Eight trials reported adverse events, and found no adverse events directly resulting from either IMT or the comparator interventions.
What is the current guidance?
2003 NICE guidance on pre-operative testing recommends that lung function tests are considered for people who have a chronic condition, like asthma or chronic obstructive pulmonary disease that may affect their recovery. There is no specific mention of pre-operative respiratory rehabilitation. An update of NICE’s 2003 guideline was published in March 2016.
What are the implications?
Although this review indicated that IMT appears to have a beneficial effect on the risk of some post-operative pulmonary complications (PPCs) in people undergoing heart or major abdominal surgery, the underlying evidence was of insufficient quality to be certain about the magnitude of this effect.
The analysis only included three complications because there was either inconsistency or insufficient detail about how others were defined, which prevented comparisons across studies. Varying definitions also made it difficult to estimate the number of people affected. Larger, better designed trials that consistently and precisely define PPCs and patient risk are needed. None of the included studies reported on costs of the interventions or the hospital or community costs saved so more data is needed to inform practice.
Citation and funding
Katsura M, Kuriyama A, Takeshima T, Fukuhara S, Furukawa TA. Preoperative inspiratory muscle training for postoperative pulmonary complications in adults undergoing cardiac and major abdominal surgery. Cochrane Database Syst Rev. 2015;10:CD010356. This review was carried out by the Cochrane Anaesthesia, Critical and Emergency Care Group. The full NIHR Signal and additional expert commentary was published on 15 January 2016 and can be found here.
Commentary
Charlotte Pereira adds her view
In the UK, current practice results in the majority of patients receiving physiotherapy after major abdominal or cardiac surgery. This systematic review examines whether physiotherapists should have a pre-operative and proactive role for ‘breathing training’ to prevent respiratory complications from occurring, rather than treating them after they have happened (responsive service). Although this review highlights the evidence is not strong (due to bias and small sample size), it does suggest there may be benefits from using inspiratory muscle training in high risk patients before surgery.
This has been further supported by the work published earlier this year by Boden et al BMJ 2018;360:j5916 who demonstrated the benefits of respiratory training (education and breathing exercises) before surgery on the incidence of pulmonary complications. There were differences between the groups that need to be considered when applying these results to practice, but the findings are promising.
Current patient pathways and associated staffing models are not always set up to see patients pre-operatively. The challenge facing clinicians is to identify which patient groups would benefit from this service, creating the time to see them and demonstrating cost-effectiveness showing the long term economic value of investment in such services.
- Charlotte Pereira (BSc MSc MA FHEA MCSP) Clinical Specialty Lead – Transplantation, Royal Brompton & Harefield NHS Trust; Senior Teaching Fellow, UCL; ACPRC Surgery Champion.
Number of subscribers: 1




































