A pioneering group of physiotherapists has developed a gold standard for botulinum toxin therapy treatment, which is changing the management of spasticity. James Benson reports
For the past decade, Peter Harding, director of the physiotherapy team at the West Midlands-based practice, NPP Neuro Group, has been leading some innovative work aimed at breaking down barriers to physiotherapy becoming the go-to profession for spasticity management.
His contributions include input to an MSc module in spasticity management and injection therapy developed with Coventry University, which has been replicated at several universities including Southampton, Lancaster and London. The courses are designed to be organic so that they can adapt to changing practice, moving from muscle identification through palpation to electrical stimulation, and now teaching the use of ultrasound guided techniques. Alongside consultant neuro-physiotherapists Dawn Hicklin and Dr Cameron Lindsay and consultant musculoskeletal physiotherapist Mark Maybury, Peter has authored ‘The Botulinum Toxin Workbook (Management of Spasticity – Clinical Application and Needle Techniques for Botulinum Toxin Type-A)’.
When Peter started looking at the role of physiotherapists, managing the spasticity pathway in the early 2000s there was a very small number of AHPs administering botulinum toxin.
He explains, ‘My interest in spasticity management really became focused when I was studying for a MSc in neuro rehabilitation while working as a senior physiotherapist at Queen Elizabeth Hospital in Birmingham. My dissertation aimed to ascertain the best way to manage spastic equinovarus in acute head injuries using botulinum toxin and soft and scotch casting. The results of this have been written into a protocol for acute head injury units. It is now generally accepted that spastic equinovarus as a result of acquired brain injury is preventable with careful forward thinking management.
‘During my studying it occurred to me that physiotherapists were in a pivotal position to manage a spasticity pathway including the administering of the botulinum toxin but at the time only three allied healthcare professionals were injecting and under close supervision’.
Several years on and following the CSP’s success in gaining full prescribing rights for physiotherapists, the profession has hugely influenced the change in spasticity management. Hundreds of physios in the UK are currently proficient in carrying out the injections and many are also running autonomous spasticity management clinics.
Three years ago Peter’s NPP team started working with the Royal Orthopaedic Hospital in Birmingham to manage their cerebral palsy adolescents as they transitioned to adult services. This is predominantly a spasticity injection service using Botulinum Toxin-A, but from this clinic patients can access other services that may be required to manage their limb spasticity.
Attracting wider attention
While it is managed by physiotherapists, the clinic is staffed by a multi-disciplinary team (MDT) that includes doctors, physiotherapists, occupational therapists and orthotists. The difference from most NHS spasticity clinics is that all of the clinicians are able to triage to a similar high standard and then proceed to injection therapy all in the same appointment slot. Nearly one million of units of Botulinum Toxin-A have been administered safely and effectively in the Royal Orthopaedic Hospital clinics (clinical audit results 2018) and it has grown from treating 12 patients a month to more than 60. On the basis of this work, the toxin licence is being changed to state that suitably qualified AHPs can inject Botulinum Toxin-A. The NPP team has recently widened its work to include another spasticity management clinic that will serve children from two years of age until they are adolescent, at Russells Hall Hospital, which is part of the Dudley Group NHS Foundation Trust.
This success has started to attract wider attention. In 2018, Peter delivered the keynote speech at the Toxins 2018 Nordic Congress (sponsored by Ipsen Ltd) in Sweden, and his team has been invited to attend the 2019 conference and to start sharing skills of injecting Botulinum Toxin-A using ultrasound guidance with physiotherapists across some of the Nordic nations, including Sweden, Denmark, Norway and Finland. This is work in progress and likely to be in Sweden later this year. Several governments and health boards in these countries have specified that these techniques should be part of physiotherapists’ and other health care professionals’ skill set.
Peter is encouraged by the progress made over the past decade. He says, ‘Increasingly I envisage that more and more areas of rehabilitation will be therapy led, especially as physiotherapists can now prescribe - with the requisite training. We have already seen this change within spasticity management clinics, and I can only see the role of neuro-physiotherapists growing.’
- Physiotherapists are perfectly placed to manage spasticity and should be striving to lead in the area across all neurological conditions.
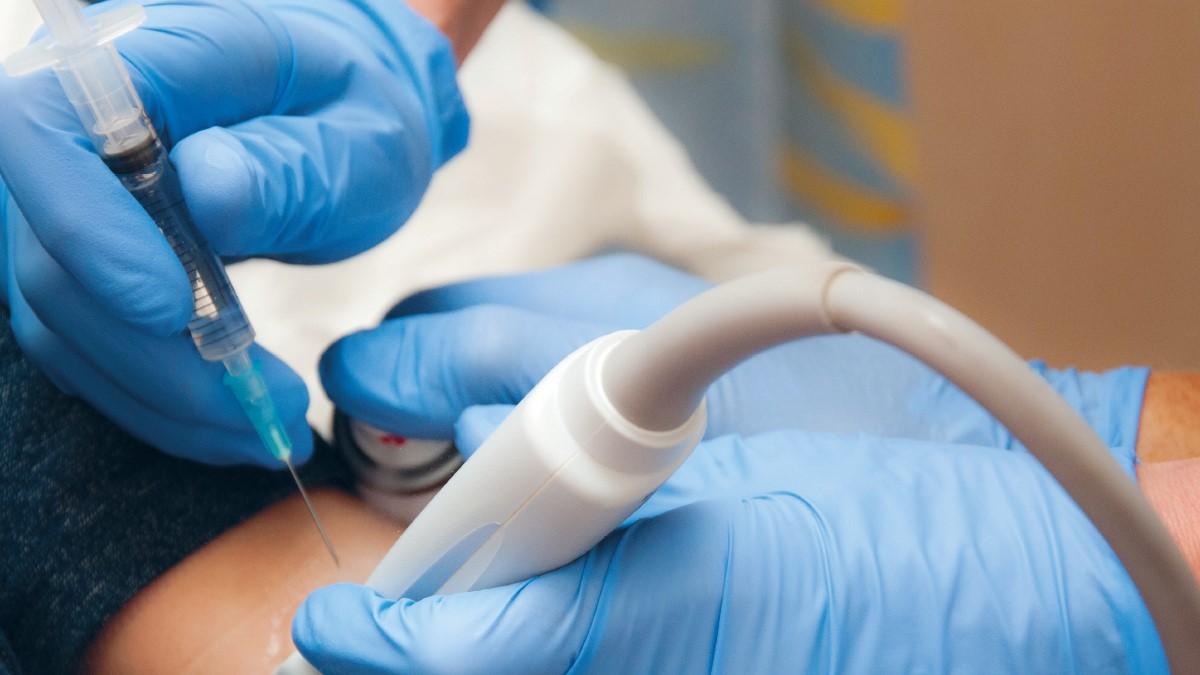
- The use of ultrasound is becoming an essential skill within many areas of practice and should be used more widely at universities to enhance anatomy knowledge and application.
- CSP members can access free educational programmes such as the Continuation of Learning to Improve Management with Botulinum toxin (CLIMB programme).
- Peter Harding is the director of the physiotherapy team at the West Midlands-based NPP Neuro Group which provides both adult and paediatric neuro rehabilitation services to the NHS.
- James Benson is a clinical specialist physiotherapist and CSP Council Member.
Number of subscribers: 12




































